CONCIERGE MEDICAL CARE
AUSTIN | DRIPPING SPRINGS
ESCAPE THE BROKEN HEALTHCARE SYSTEM
CONCIERGE MEDICINE BUILT FOR HIGH-PERFORMING ADULTS WHO REFUSE TO SETTLE FOR RUSHED, REACTIVE CARE
Dr. Peter Cashio and the Code 1 team provide direct access, full-spectrum care for your body, mind, and performance -- without insurance interference, wait times, or hidden costs.
Dr. Cashio creates a personalized protocol, built on hundreds of successful transformations — designed to reboot your health, clarity, and energy from day one.
A DOCTOR THAT KNOWS YOU LIKE A BROTHER - BUT COACHES LIKE A MARINE
Dr. Cashio knows that success depends on knowledge, trust, and accountability. The knowledge is a given, and we know that you'll come to trust our guidance.
Marine Corps veterans like Dr. Cashio know that accountability is the critical piece that creates success.
It works for the Marine Corps and it will work for you.
Success Story “I’m stronger at 47 than I was at 22.”
(Opens a separate sign up form)
OR
(Chat with our Team)
< 5 min
To see your doctor (no waiting)
< 1 hour
To hear from your doctor
30 days
To improved health & energy
90 days
To HUGE health improvements
100%
Unique, personalized
health recovery plans
650+
Happy, transformed lives
"MODERN MEDICINE" SUCKS
IS THIS YOUR EXPERIENCE WITH MODERN MEDICINE?
10-minute visits and endless referrals?
Feeling dismissed, rushed, or uninformed?
Being told that your labs are “normal" or "healthy," but not feeling normal or healthy?
Half-baked advice like “just eat better” or “walk more," or "try lifting weights"?
Being told that "You're just fine"?
BUT YOU’RE NOT FINE.
IN FACT, YOU'RE FAR FROM "FINE"
You're tired and fog-brained.
You're out of shape and hate looking in the mirror.
You feel like you're falling behind.
Nothing seems to work.
It seems like no one is actually listening
CODE 1: BUILT FOR YOU, NOT INSURANCE COMPANIES
AT CODE 1 CONCIERGE, YOU'LL GET
Deep health evaluation — bloodwork, hormones, diet, fitness, stress
Unlimited visits and direct access to your physician
Action plans built around performance, longevity, vitality, and your goals
Concierge care for both men and women — including hormone optimization (if appropriate)
Revitalization systems that actually work
Advanced analytics and treatments
The gift of time
THE BOTTOM LINE
You don’t need another rushed visit.
You need a comeback plan — designed by someone who knows your body and your goals
That's exactly what we'll build — together

(Opens a separate sign up form)
OR
(Chat with our Team)
REAL PATIENTS | REAL CARE | LIFE CHANGING
From tired, overweight, and ignored… to confident, empowered, and living life
"I' just feel so taken care of"
"You know, with Dr. Cashio, it's more of, “let's take a step back. Like, who are you? What are your goals? Let's take an assessment. Let's do the blood work. And let's kind of not just rush you out of here. Let's have a long-term relationship. Let's make you as healthy as possible."

"I've had more personalized care in the past month than I've had at any previous physician prior to this."
""Actually, he went to bat for a medicine that my insurance copany denied. He appealed it. That's the first time that a doctor has ever done that and it has made a difference. Now I am able to get this medicine on my insurance. I appreciate Dr. Cashio and all that he has done for me."

"My life changed forever"
"Interesting thing to me was how you approached it. Let's be practical. Let's make these life changes rather than treating something with just medicine. You know, medicine has its place and there is a need for the medicine, but it's not everything. And that collective holistic view of caring for me and my body was the first time I'd ever experienced something like that."
| The Transformation
- Challenges: Overweight, Low T, & no drive
- Weight (start): 214 lbs
- Weight (end): 181 lbs
- Now: Excellent health, massive confidence, financial success
- Success Event: Climbing Mt. Rainier in glacier conditions

"Doc, you saved my life"
"His approach is just totally unique. It's totally different. Someone that genuinely is invested. There just isn't anyone else that does that in standard medical practice."
| The Transformation
- Challenges: Overweight, Low T, fatigued, & falling behind
- Weight (start): 298 lbs
- Weight (end): 237 lbs
- Now: Confidence, energy, new friendships, great marriage
- Success Event: Completing a grueling, 100 mile bike race

"I' just feel like I'm dialed in"
"You know, with Dr. Cashio, it's more of, “let's take a step back. Like, who are you? What are your goals? Let's take an assessment. Let's do the blood work. And let's kind of not just rush you out of here. Let's have a long-term relationship. Let's make you as healthy as possible."
| The Transformation
- Challenges: Fatigue, poor exercise tolerance, Low T
- Weight (start): N/A
- Weight (end): N/A
- Now: ⬆⬆ Energy, ⬆ Performance, dialed-in, proactive health
- Success Event: Running a half-marathon

"I've hit new records"
""Between the medical attention that he gave me and doing the cold plunges, I not only healed, I was able to actually go back to the gym and become a bodybuilder. I've hit new records where doctors told me you'll never lift weights again."
| The Transformation
- Challenges: Chronic back pain, Low T, Low energy
- Weight (start): 188 lbs
- Weight (end): 204 lbs (lean muscle)
- Now: Rare pain, ⬆ Energy, Bodybuilder
- Success Event: Making massive gains in lean muscle mass

(Opens a separate signup form)
Elite health — founded by a Marine, forged in the ER, built on science
Medicine for Men & Women who want their health back — and won’t settle for less.
(Opens a separate signup form)
Start Your Amazing Journey
3 steps | One doctor | Life-changing results.
Click "Join Today"
1 click towards a healthier you
Fill out the Form
Short and Focused. 😀
We'll call ASAP
New patient appointments in ~ 1 week
(Opens a separate signup form)
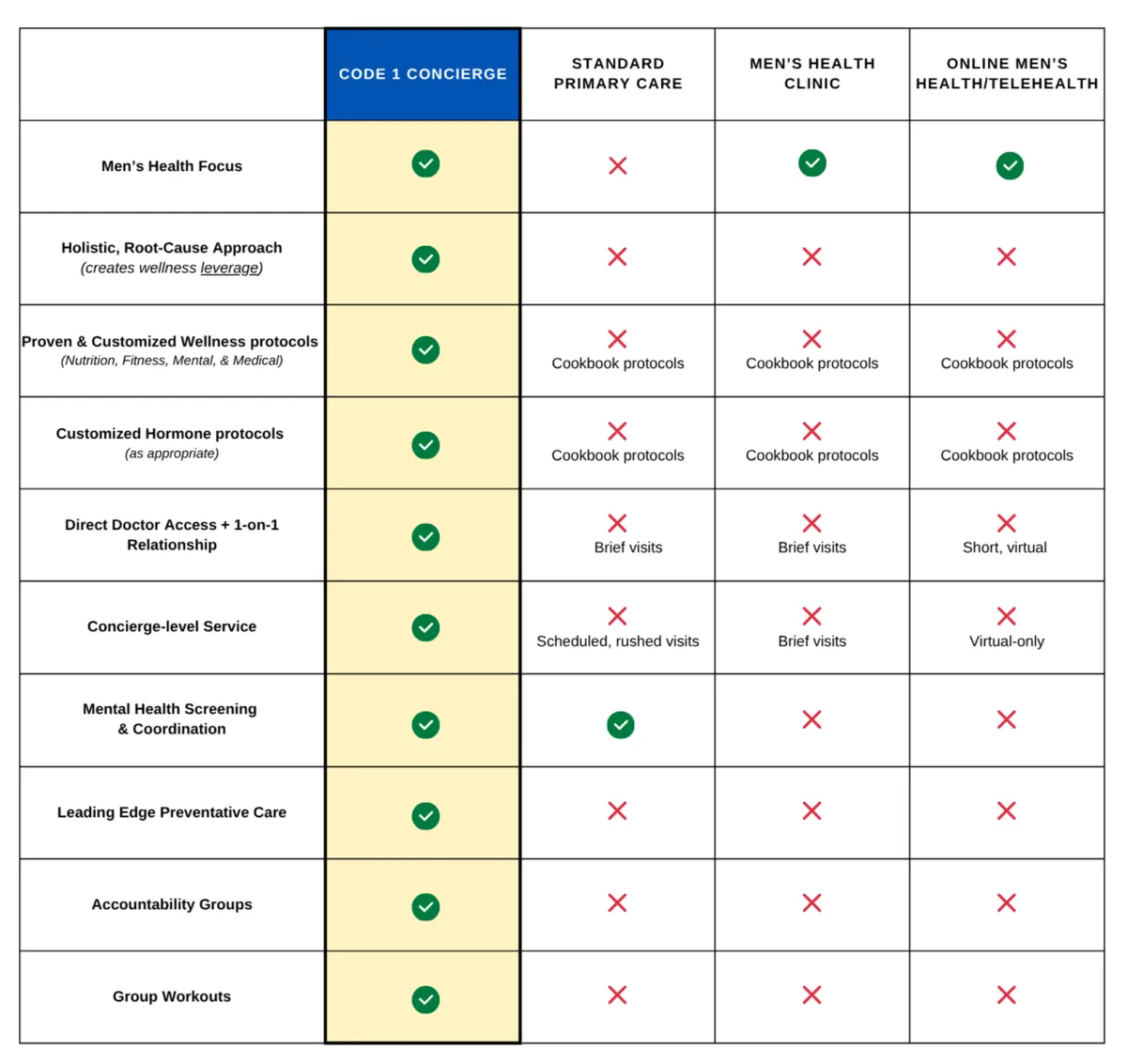
Services Offered

VIP-LEVEL CONCIERGE MEDICINE
The Elite-level care that you deserve

REFORGED WEIGHT
LOSS PROTOCOL
Reshape Your Body. Restore Your Power.

APEX TRT PROTOCOL
Lead Your Life with Strength, Clarity, and Fire

ATHENA HRT PROTOCOL
Lead life with renewed power, vitality & energy

ADVANCED LAB ANALYSIS
Unlock your body's hidden secrets & take control

VITAL EDGE
PEPTIDE PROGRAM
Targeted, precision solutions customized for your needs
MEMBERSHIP

$249/mo*
INCLUDED SERVICES
1.5 hr Initial Physician Consultation
VIP Lab Analysis & Wellness REVIEW
1 x InBody Body Composition Scan per month
Bespoke Roadmap for Your Future Health Success
Direct Physician Access
Intensive, 12 week onboarding process
Standard Code 1 Patient Benefits
Appointments: Same or Next Day
Appointment Length: 30 min - 1 hour
Urgent Care service (as appropriate)
Ultrasound: Advanced Diagnostics
Procedures: Many advanced procedures done in-clinic
Standard Cardiovascular Screening
EKG
Ankle Brachial Index
Cardiac Ultrasound (basic)
APEX Testosterone Replacement Therapy Protocol (included, if appropriate)
Mental Health Screening & Coordination
AVAILABLE SERVICES
AFFORDABLE, IN-HOUSE LABS Via Access Medical Labs
VITAL EDGE Peptide Program (BPC-157, Sermorelin, etc)
REFORGED Weight Loss Program (including peptides)
PERSONAL TRAINER Program
NUTRITION COACHING Program
IV HYDRATION THERAPY
*ENROLLMENT FEE
*ALL MEMBERSHIPS REQUIRE A ONE-TIME, NON-REFUNDABLE $1,999 ENROLLMENT FEE.
Meet Dr. Cashio
Peter Cashio, MD MS
—20+ Years in Medicine
— Emergency Medicine & Critical Care
— MS in Developmental Biology (genetics)
— USMC Intelligence Analyst
BRIEF BIO
Cajun-born, grew up in Texas and Southern California.
US Marine Corps veteran, former USMC Intelligence Analyst, Ninja (yes, really!), lived in Okinawa, Japan for two years.
UT Austin graduate (“Hook ‘Em”), UT Houston/MD Anderson for graduate school in developmental biology & genetics (Drosophila melanogaster - best model organism ever), UT San Antonio for Medical School, and Board certified Emergency Physician (Go ‘Hoos!).
15+ years as an Emergency Medicine physician (with lots of critical care). I founded Code 1 Concierge Care in Dripping Springs, TX because I felt like there had to be a better way to care for patients.
I love sports with my boys, Japanese culture, powerlifting, running, science-fiction, firearms, marksmanship, getting strong and fit, first-person shooter video games (Halo, Battlefield, COD, etc), and taking care of other veterans.
EDUCATION
Undergraduate: UT Austin (2000)
Master of Science: UT Houston/ MD Anderson Cancer Center (2005)
Doctor of Medicine: UT Health Science Center at San Antonio (2009)
Residency: University of Virginia, Charlottesville, VA (2012)
PODCAST APPEARANCES
My DPC Story | Episode 143
Dream Catalyst | Episode 11
The Amy Edwards Podcast | Episode 107
OUR TEAM

Peter Cashio, MD MS

Matthew Perdue, PA

Rebecca, RN

Jenna, RN

Sandra Wilson
Frequently Asked Questions
You have questions. We have answers.
Do you treat women? Or is the practice for men only?
We love caring for women and we understand their needs too.
How does concierge medicine work?
It's a monthly MEMBERSHIP based service. You pay one monthly fee which covers:
-- Unparalleled treatment
-- Cell phone access to your doctor
-- All doctor's visits
-- All telemedicine visits
-- Minor urgent care needs
-- All referrals
-- If sent to the ER or admitted, We will closely coordinate with the ER or hospital staff.
Plus significant savings on:
-- Labs
-- Procedures such as IVs, joint injections, lesion removals, biopsies, fracture management, and so on.
VISITS: How quickly can I get an appointment?
New patients: Can usually be seen within 7-10 days.
Urgent issues: Same or next-day
Non-urgent issues: usually 1-3 days
INSURANCE: Does Code 1 take insurance?
NO
Accepting commercial insurance means increased costs (staff, equipment, software, and time) and decreased time for your needs.
-- Moreover, it causes you more pain:
-- Surprise billing for non-covered costs
-- Hundreds to thousands in out-of-pocket expenses
-- Delays in care.
Our experience shows that you are happier and you get better care if we avoid the insurance company altogether
INSURANCE: Does Code 1 replace insurance?
NO
Serious accidents and medical situations happen. In those cases, you will still need insurance in order to cover:
-- ER Visits
-- Hospitalizations
-- Many specialist visits
-- Outpatient procedures (colonoscopies, sleep studies, etc).
-- Medications
Nowadays, there are options other than traditional insurance.
Our friends at Ochna Health (in Georgetown, TX) were kind enough to put together this helpful guide to what are called Health Sharing plans.
These are non-insurance based groups that agree to cover medical costs (subject to clear rules). My own family is covered by one of these plans, and depending upon your family’s situation, these can be a great choice for catastrophic care.
Note: Code 1 Concierge Care is not affiliated with these organizations.
-- Link: https://ochnahealth.com/wp-content/uploads/2023/07/Health-Cost-Sharing-v2023.pdf
INSURANCE: I have insurance. How does that work?
Ok. So how does this work if I have insurance?
Simple
1️⃣ Join the Code 1 Concierge Care family
2️⃣ Change how you think about health insurance:
A) Transition to a catastrophic/high-deductible insurance plan, which typically have VERY LOW premiums with HIGH deductibles.
OR
B) Switch to a health sharing program like Zion, Samaritan or Sedera. Immediately save:
-- Hundreds per month
-- Thousands per year
OR
C) Continue on with your current insurance plan.
3️⃣ Use your coverage (whichever flavor) for:
-- ER Visits
-- Hospitalizations
-- Some specialist visits
-- Medications
-------------------------------------------------
A CRAZY FACT ABOUT HEALTH INSURANCE
-------------------------------------------------
❗️Using your insurance is like constantly using your auto insurance. Eventually, your rates will increase.
LABS: How do labs work?
1️⃣ Decide if you want to pay cash or use your insurance for labs.
2️⃣ Cash labs:
-- We will draw the labs in our clinic
-- It is fast, comfortable, and usually much cheaper than using your insurance or a commercial lab.
3️⃣ Insurance labs:
-- We’ll fax an order to whichever CPL lab location is closest to you.
-- When you’re ready, go to that lab and have your labs drawn.
-- We email or call you with the results within 2-3 days of receiving them
IMAGING (X-rays, CT scans, MRIs, and Ultrasound): How does that work?
Orders for these studies can be sent to any Austin Radiological Association center or any other radiology center that you choose.
✅ There is always a cash-based option, even at ARA.
✅ You can use your insurance if you desire.
REFERRALS: What if I need a referral to a specialist?
Code 1 Concierge physicians can refer to specialists like any other doctor.
⚠️ Some HMO insurance plans require that you have this referral/order sent by your HMO primary care doctor. If that's the case for you, let us know and we can work to make that as painless as possible.
SPECIALISTS: Can Code 1 replace a specialist?
NO
Get In Touch
Email: [email protected]
Address
14101 Hwy 290W, St. 400A, Austin, TX 78737
Office Hours
Mon – Fri 8:30am – 5:00pm
Saturday, Sunday – CLOSED to the public
Phone Number:
512-894-5050

© 2025 Code 1 Concierge Care - All Rights Reserved
512-894-5050